Two years ago, I gave birth to a beautiful baby boy at home. Two days after his birth, we ended up in the hospital for him to undergo surgery to repair a congenital malformation. You can read the full story of that adventure here. Today marks the second anniversary of his life-saving surgery. Yesterday evening as I held this little miracle as he fell asleep, I thought about what life would be like if he had not survived the ordeal.
We are fortunate enough to have two other beautiful children, whom we love and cherish and who would have kept us busy. Life would have gone on and we would have reached some sort of new normal, but there would always be an emptiness lingering in the background if little B was not around. His impish antics and contagious grin make him a continual source of humor and joy in our family. Although we would not know what we were missing, our life would be less colorful without him. For this reason, I am so thankful to the hospital doctors, nurses and staff as well as the advances in medicine and our access to it which made his recovery possible. However, my opinion of hospital stays and medical interventions are not always so positive.
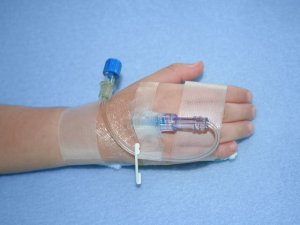
We chose to have Little B at home because I did not enjoy my experience delivering at hospitals with the first two children. For me, the time constraints that are put on labor in the hospital made me feel under pressure. I am also not a big fan of needles being stuck into my vein and then feeling fluid being shoved in there. It’s weird and it stings, and I really, really, really don’t like it; however, testing positive for Group Beta Strep in both pregnancies meant the IV was non-negotiable because they had to administer antibiotics every four hours. This was also a source of concern for me, since with my second child, I was in labor for over 30 hours, which meant I was given a lot of antibiotics. I am a big fan of antibiotics for treating infections, but they do have adverse affects especially in such high quantities. I did not realize that they had to be administered until the baby was delivered, and when I asked how many doses they were going to give me, the nurse called in the head nurse who told me that unless I wanted to risk my baby going blind, I would happily accept the antibiotics and not make a fuss about it. At least, that’s what I remember her saying in my labor haze. She may not have used those exact words, but whatever she said, she wasn’t very compassionate about my concern. The other enemy to labor for me was the fetal heart monitor, which at both hospitals where I delivered was required to be attached to my abdomen for 20 minutes of every hour. That meant that in the height of labor while I was trying to manage the pain of contractions, I had to lay on my back on the bed and have two itchy velcro straps placed around my abdomen. The sensation on my skin as well as the need to lie still in order to get a good reading was so annoying to me to deal with while I was trying to get in the zone and breathe through the pain. All I wanted to do was stand in the hot water of the shower, not lie on that bed of pain, but every 20 minutes I had to leave the comfort of the water and get back in that bed while the nurse fussed over me and put on the contraption of torture. Finally, came the pitocin.
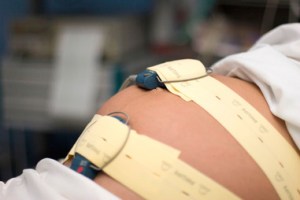
With my first child, I did not know what pitcoin was. I labored for 12 hours without an epidural before the doctor said that it was necessary to administer something to move things along. I agreed because she was the doctor and she must know best, right? Nevermind that it was 3p on a Friday, and she was probably more concerned about getting home at a reasonable hour than about what was best for me and my baby. When she said the contractions would get stronger and closer together, I said I wanted the epidural now. With our second child, I put off suggestions of pitocin as long as I could, but after 24 hours the staff became pretty adamant. I agreed to the pitocin as long as the nurse agreed to turn it off once the contractions became stronger and more consistent. She agreed, but she must have had her fingers crossed behind her back, because when I told her after an hour and a half that it had worked and now I was in full labor and it was time to turn it off, she said she couldn’t do that. I made some sort of noise of displeasure from my perch in the bathroom. Luckily, she was standing out in the room with my doula, otherwise she might have gotten decked in the face for what she said next, which was, and I quote this time because the words are etched into my brain in blood, “She does know that labor hurts, right?” After that I yelled something at her involving the f word and the next thing I know she was turning off the pitocin. An hour later, I transitioned to 10cm, and two hours later a beautiful bay girl was born. After that experience, I decided that when we had another, I wanted to plan a home birth. I am so glad that I did, because with Little B’s birth we could not have asked for a better experience.

Little B’s birth from onset to delivery was 10 hours and required none of the interventions or contraptions that the other deliveries did. I believe that the delivery went more smoothly because I felt safe in my own home, in a way that I did not feel in the hospital. I labored with a midwife, her assistant, an experienced doula, and my husband. The midwife came with the capability to administer an IV or oxygen, but left those tools out in the kitchen away from the room where I labored. We lived two miles from the hospital should the need to transfer arrive. We planned for emergencies, but we didn’t expect them at every turn. In addition to a smoother delivery, recovery was much more comfortable as I did not have the late night interruptions of hospital required blood pressure checks and temperature readings. My favorite part was that my arch enemy, the IV, was nowhere in sight.
For me, my home was the best choice for that particular pregnancy because it was where I felt the most relaxed. For other women, the hospital is where they feel the safest. Some women are not bothered by the fetal heart monitor or lying down on the bed. The idea that life-saving interventions and medical staff are right on hand help them to relax and do the work of delivering their baby. This makes the hospital their best choice. It’s important that a laboring mother feels safe. Women’s bodies are biologically wired to seek a safe, secluded space for laboring. Our bodies are able to slow labor if we sense danger through the neocortex decreasing the release of oxytocin and to enter into labor when we register all as well through an increased release of oxytocin. Here is an excellent article with more detail on the subject.
My experience birthing children in hospitals as well as having a little one stay in the hospital has lead me to an interesting perspective of them: I am so grateful that they exist for when we really need them, but I wish to avoid them if at all possible. After several years, I can now say that although our hospital stays were not the experiences I was hoping for, the important fact is that they all ended in bringing home healthy babies and a healthy mama. This seems to be a recurring theme for our time here in Thailand. Many of our experiences are not what I would have chosen, but I am grateful for them anyway because they have made us stronger as individuals, as a couple and as a family.
We have been living in Thailand for 9 months now. The time has flown by, but it has been jammed full with so many issues we never would have experienced in the states. Thanks to the stability offered by our faith, new friends we’ve made and the bonds of our family of five, we’ve made it through. And, as I said, as time goes by, those issues that caused so much stress are slowly transforming us into wiser and more grateful people who earnestly long to see The Good Life realized throughout this world.
(Addendum: to be clear, I am not a nurse-hater. I love nurses. Duh! I married one. I realize that the main reason that my experiences were so challenging was due largely to the fact that hospital policy is driven by risk management. Even my husband struggled with this in the ER he worked in. I believe the nurses that served me meant well, but were burdened by the expectations of the hospital, which unfortunately were designed not to serve their patients, but to protect their assets.)
Preach it, sister!! 🙂 Love this! I love hearing happy home birth stories. I wouldn’t change my two for the world. Much for that reason, I am studying to become a birth doula to help other women have an empowering, satisfying, healthy experience.
LikeLike
Thanks, Jen. Sounds fun! I have a whole list of things I want to do in my “next life” (as in after kids aren’t so little and I have brain cells to do such things as study). Being a doula or midwife is on the list. Good job to you for tackling it now in the midst of the chaos.
LikeLike
I worked in hospitals a good portion of my life. I so dislike them- but, like you, know their necessity. I had a daughter with brain cancer and was so grateful for the people who cared (and even for the few who did not).
LikeLike
Thanks for your comment. I am sorry to hear about your daughter, but am glad that she got the care she needed. Good work starting a blog. I look forward to reading more of your thoughts. Blogging is a great way for us introverts to stick together!
LikeLiked by 1 person